Next story: When To Consider Weight Loss Surgery, Part II
Comprehensive Weight Loss Center, Part I
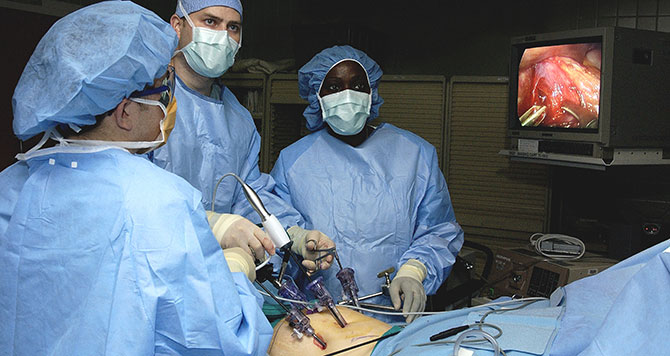
When to consider surgery
Recognizing the seeming explosion of obesity in the country during the past decade, ArtvoiceTV.com host Judy Sperry went to Buffalo General Hospital to speak with Dr. Aaron Hoffman about surgical treatments for obesity.

AV: Hello, Dr. Hoffman, can you tell us a little bit about your specialty and what the program is that you’re involved with here?
AH: Sure, at Buffalo General my partners and I, Dr. Alan Posner and Dr. John Butch run the Kaleida Health Comprehensive Weight Loss Center. People come to us who have had trouble losing weight and keeping it off; it’s not their first choice. Surgery should really be the last option.
AV: Are they referred here by their primary care doctor?
AH: We get calls from people who hear about us through word of mouth and sometimes their doctors send us patients if they have weight related health problems like diabetes or high blood pressure and surgery is the only answer to help cure them of these problems.
AV: Are patients both children and adults?
AH: We focus our practice on patients eighteen and up. We feel that adolescents are going through so many changes that it’s difficult from a surgeon’s point of view to care for adolescents, so we focus our practice on adults.
AV: Will they see a nutritionist or undergo some type of psychiatric evaluation before they begin the program?
AH: All of our patients undergo a thorough screening process. We’ll assess their health and their weight and we’ll have them screened by the nutritionist and usually a physical therapist, as well. Also, all weight loss surgery patients have psychiatric evaluations before they undergo surgery. We want to make sure that they understand that while weight loss surgery is very safe, that this is a big step towards their health. They have to have the capacity to make the decision to undergo an elective surgical procedure.
It’s also important that people know this is not a quick fix and this is in many ways is a marathon rather than a sprint.
AV: What are the criteria for surgery?
AH: We use the National Institute of Health’s criteria guidelines. In a nut shell that means patients need to see if their Body Mass Index (B.M.I) makes them large enough for weight loss surgery. There are a number of websites for calculating your B.M.I.
Someone that needs to lose five or ten pounds before a wedding does not need surgery. People who have surgery are usually sixty to a hundred pounds overweight.
If their B.M.I. is between thirty-five and forty and they have major health problems like sleep apnea, diabetes and hypertension then they’re eligible for surgery. If their B.M.I. is over forty but they don’t have any other health problems they are still are eligible because of being big enough for weight loss surgery. Most insurance companies follow these same guidelines and in fact pays for the surgery.
AV: What are the surgical procedures you use?
AH: There are three procedures that we do and all of them are laparoscopic. Laparoscopic surgery is abdominal surgery but we use small cameras and small instruments so we don’t have to give the traditional open operation.
The tried and true is the laparoscopic gastric bypass, a procedure where we give patients a small stomach by stapling and cutting their existing stomach and making it smaller. Then we bring up a loop of their small intestine to the new stomach and this works in two ways. They feel full on a small amount of food and with the rearranging of their intestines and slight malabsorption, they don’t absorb all of their calories.
This is the oldest procedure. It was first described in the sixties but really took off in the early nineties when surgeons were able to do it using cameras, which is what we use.
The other two procedures are the laparoscopic adjustable gastric band, which some people refer to as the “lap band.” That’s simply putting a silastic balloon around the upper portion of the stomach, making people feel full on a small amount of food. But because we don’t cut or alter the intestines or the stomach it’s potentially reversible unlike the bypass, which is permanent. So the band is a lot safer because we’re not cutting any organs out and we just wrap it around the stomach to give them a sensation of fullness. The weight loss is a little bit slower as you could imagine with the band but it’s a lot safer.
The third and newest procedure that Dr. Posner, Dr. Butch and myself perform is called the vertical sleeve gastrectromy and this is where we reshape the stomach in such a way that you feel full on a small amount of food but we don’t have to rearrange the intestines so you don’t have any problems with malnutrition or vitamin deficiencies like you do with the bypass.
AV: Are these considered to be minimally invasive procedures?
AH: All the procedures that we do are minimally invasive.
AV: And what is the recovery time for these patients?
AH: Patients stay an average of less than two days in the hospital. The band patients usually go home after one day and the bypass usually goes home after two. About eighty percent of our practice is lap band now. Two years ago we were about eighty percent bypass, but the lap band has had great success and for the majority of our patients the lap band is their choice.
But for certain patients, and we can discuss this in the office individually with the patient, certain patients may benefits from the old-fashioned bypass, or the sleeve. The problem with the sleeve right now is because it’s the newer procedure they haven’t quite accepted it yet as a primary procedure. Insurance right now doesn’t cover the majority of sleeve gastronomies.
AV: Do you follow the patient after the surgery?
AH: In Bariatric surgery we follow the patients long term. We’re kind of their primary care doctors for weight loss. All of our patients have to be educated about what to eat and what not to eat. And occasionally through education some patients say ‘I never really understood how to eat right.’ That’s the reason we call it the Comprehensive Weight Loss Center, because when possible we also instruct patients on diet and exercise so they don’t have to have surgery. If the patients are doing great and losing weight without surgery, patients stay on the non-surgical track, and we’re happy if they can do that.
AV: Would you recommend that couples do this together?
AH: I’ve been fortunate enough to operate on about thirty married couples and about fifteen members of extended families. I’ve noticed that people that go into weight loss, or exercise together, tend to do better than someone who is doing it by themselves. I think this is true because they support each other and they bring healthier food into the house, so the whole family benefits.
—Interview for Artvoice by J.S.
In addition to speaking with Dr. Aaron Hoffman, Judy Sperry also interviewed Dr. Alan Posner who founded the Comprehensive Weight Loss Center. Read Part II of this story here.
blog comments powered by Disqus|
Issue Navigation> Issue Index > v9n37 (Health & Fitness Issue, week of September 16) > Comprehensive Weight Loss Center, Part I This Week's Issue • Artvoice Daily • Artvoice TV • Events Calendar • Classifieds |









 Current Issue
Current Issue